- Male
- 29 Years
- 22/01/2025
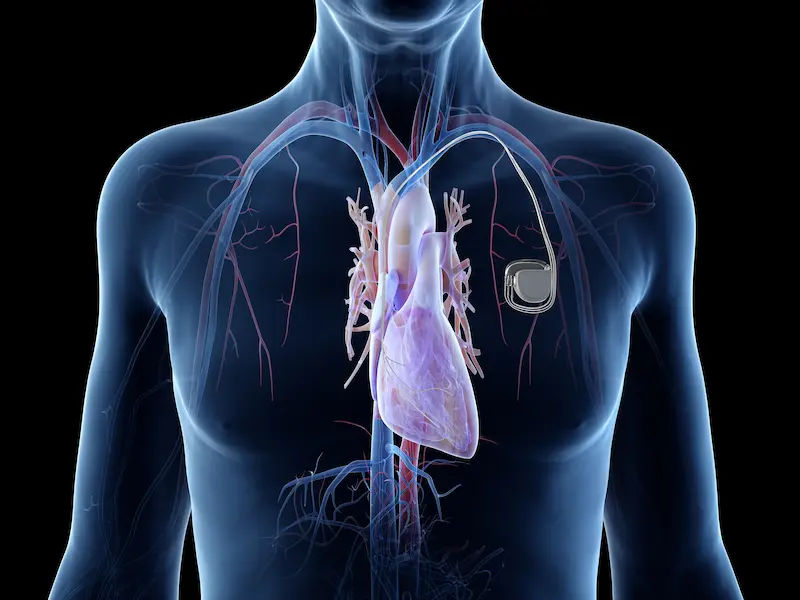
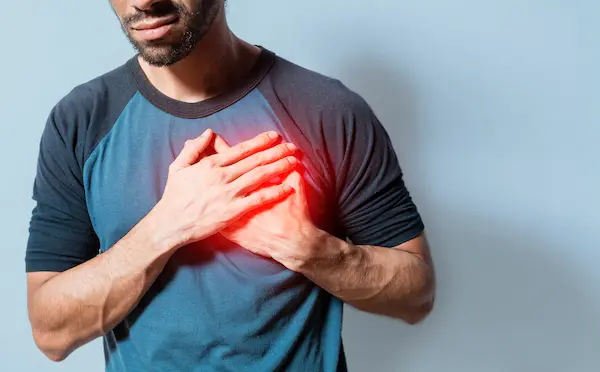
I've been having this pain in the heart area of my chest for over three months now, and it happens about twice a week. I haven't been doing any kind of exercise recently. I'm starting to get really worried about it. Could this be something I should be concerned about? What might be causing this, and what should I do?
More Cardiology Health Queries
View allI'm really worried because every time I feel stressed, I get chest pain and end up panicking. I rush to get an ECG and 2D echo done, but it's always normal, which is honestly exhausting. I'm scared it's something serious like a heart attack, but then the tests say otherwise. What should I do? Any advice would be appreciated.
To help manage your symptoms, you can try taking a medication called **Propranolol**. This is a beta-blocker that can help reduce the physical symptoms of anxiety, such as chest pain and palpitations. The usual dosage for Propranolol in such cases is 20-40mg taken 2-3 times a day. Additionally, you may benefit from an anxiolytic medication such as **Lorazepam** to help with acute episodes of anxiety and panic. The typical dosage for Lorazepam is 0.5-2mg taken as needed for anxiety symptoms. It's important to also consider non-pharmacological approaches to managing stress, such as relaxation techniques, deep breathing exercises, regular physical activity, and seeking support from a therapist or counselor. Remember to consult with your healthcare provider before starting any new medication.
Answered by 1 Apollo Doctors
My dad experienced some chest pain and his blood pressure was pretty high last night, so we decided to get an ECG done this morning. The results are in, and they mention something about a non-specific T wave abnormality. I'm trying to figure out what that means exactly. Any chance you could help us understand this a bit better?
See a specialist for accurate diagnosis and targeted treatment.
Answered by 1 Apollo Doctors
I'm on Amlovas 5 mg for high blood pressure, but it's causing me acid reflux and chest pain. Is it okay if I stop taking this medication?
No, u have to continue BP medications life-long.
Answered by 1 Apollo Doctors
Disclaimer: Answers on Apollo 247 are not intended to replace your doctor advice. Always seek help of a professional doctor in case of an medical emergency or ailment.